Co-authored with Dr Kate Whimster, ND
Gluten awareness has greatly increased in the last decade. This has come with great progress for individuals who must live gluten-free. The number of individuals going gluten free has increased. Not all of them who have chosen to go gluten-free are celiac, so what’s the rational? There are more reactions to gluten then that of the most known celiac diagnosis. An emphasis on celiac and the symptoms associated with it as well as different types of gluten reaction will be explored.
In a past article, we discussed the difference between food sensitivity, allergy and intolerance. I highly recommend you review that article prior to reading this one. Despite my best effort to avoid technical terms. Some of the concepts of this article build on that article.
What do anemia, diarrhea, constipation, hypothyroidism, osteoporosis and a type 1 diabetes trigger have in common? They can all be signs or symptoms of some type of reaction to gluten. Over 100 symptoms have been to varying degrees associated with gluten. This is why this topic is vast and confusing.
What is gluten?
Gluten is a protein found in all types of barley, rye, wheat and spelt. An acronym to help you remember is B.R.O.W.S: Barley, Rye, Oats (debatable), Wheat and Spelt. Oatmeal is sometimes included due to risk of contamination. It is often farmed, transported and/or package in factories that also have gluten containing grains. A recent study suggest most individuals with celiac can tolerate uncontaminated oats well (Kemppainen et al, 2007). Extra precaution can be taken by purchasing Gluten-Free Oats which means careful attention to potential contamination has been considered. An example of this is Bob’s Red Mill Gluten-Free Oats.
3 types of Gluten reactions.
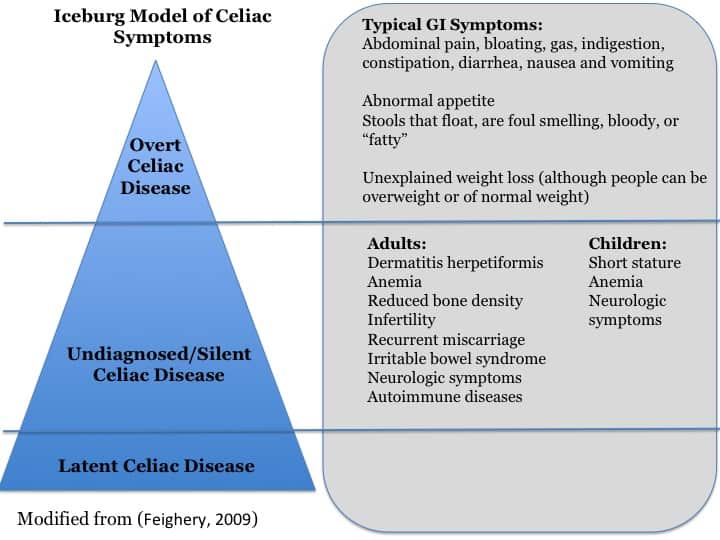
Celiac Disease is an autoimmune condition against the cells of the small intestine triggered by the ingestion of gluten containing grains. Celiac disease is the best understood gluten reaction.
One in every 133 healthy people have celiac disease. In individuals with typical celiac symptoms 1 in 56 people have celiac disease. In people with a family history of celiac disease 1 in 22-39 have celiac disease. Sixty percent of children and 41% of adults diagnosed during the study had no symptoms (Fasano et al., 2003).
The average length of time it takes for a symptomatic person to be diagnosed with celiac disease in the US is four years; this type of delay dramatically increases an individual’s risk of developing autoimmune disorders, neurological problems, osteoporosis and even cancer (Green et al., 2005).
Celiac disease is associated with greater risk of additional autoimmune conditions. The more delayed the diagnosis the greater the risk. Those diagnosed with celiac disease between 2-4 years of age had a 10.5% chance of developing an autoimmune disorder. This incrementally increased by age of diagnosis. Those diagnosed at the age of 20 years or older had a 34% chance of developing an autoimmune disorder. Additional findings show that the later one is diagnosed, the more likely he or she is to develop an autoimmune condition (Ventura, 1999).
The difficulty with celiac is that symptoms can greatly vary from typical GI symptoms to an atypical form that presents with no gastrointestinal symptoms (Sanders, 2005).
Individuals diagnosed with Celiac’s must follow a strict gluten-free diet to avoid the autoimmune destruction of there small intestine and the consequential immune and metabolic consequences. The first step to celiac diagnosis involves an in office blood test. If positive a colonoscopy of the small intestine may be performed to visualize the current damage.
Wheat Allergy is an IgE antibody mediated immune response to gluten.
These are your typical food allergy type reactions. They can vary from mild itchy skin, swollen eyes to potentially life threatening difficulty breathing. What is intriguing about this food allergy is that in some individuals with a wheat allergy, consuming wheat prior to exercise can induce anaphylaxis reaction. Following a gluten-free diet is required.
Gluten Sensitivity is defined as every other reaction to gluten.
The definition of gluten sensitivity is broader than the definition described in my article food sensitivity, allergy and intolerance. The simplest definition is all reactions triggered by gluten exposure and alleviated by gluten withdrawal. The difficulty with the research on gluten sensitivity is that the symptoms are not very predictable. Some, individuals with gluten sensitivity can experience mild to severe digestive complaints to no digestive symptoms at all. Others experience fatigue, migraines and the list goes on. If it doesn’t always look the same how can you diagnose it? It is a diagnosis of exclusion. When celiac and Wheat allergy have been ruled out and an evident reaction to gluten is seen, it is labeled gluten sensitivity. Despite it not being associated with the same risks of a celiac diagnosis, symptoms can be quite severe and debilitating.
What is it about gluten that it can be so ruinous for so many people?
“Possibly, the introduction of gluten-containing grains, which occurred about 10,000 years ago with the advent of agriculture, represented a “mistake of evolution” that created the conditions for human diseases related to gluten exposure…. a number of in vitro studies have confirmed the cytotoxicity of gluten’s main antigen, gliadin (Sapone, 2011).”
The truth is we don’t really know. We are simply realizing that many individuals are adversely affected by gluten in different ways. It’s really hard to know why our body seems to react to this protein differently… it just seems that in a great proportion of us it does.
What’s the bottom line?
- If you suspect you may be having a negative reaction to gluten in your diet never eliminate it until you have had a proper work up. I can perform a quick in office celiac test that will indicate if you have some of the blood markers for celiac. If you eliminate gluten from your diet the test is no longer valid.
- Once you have ruled out celiac, a strategic elimination and challenge diet can help assess the influence it has on your health.
- Do you tolerate gluten well? There may be no need to go gluten free although I still recommend exploring non-gluten containing grains to increase variety in your diet.
- For more details visit the 4R GI restoration program. Strategically and carefully understanding if foods may or may not be contributing to your symptoms is essential to the path of optimizing your health.
- Here is a gluten free resource guide.
Do you have a story to share relating to gluten? Please comment below.
References:
Feighery. Fortnightly review: coeliac disease. BMJ (1999) vol. 319 (7204) pp. 236-9
PubMed Health. Celiac Disease- Sprue. (2010).
Image Credit: Henry Gavamaro